Freshman nursing student Jillian Bernier notices an anxious-looking young woman cradling a bundled-up baby at the back of the room. Across the way, a group of fellow students huddles around the bed of an infant with a racing heart.
Bernier approaches the young mom. “Are you OK?” she asks. A fellow student hands Bernier a stethoscope. “Let’s just take a look,” she says to the mom, who won’t budge. “Have you felt her temperature?” she asks, but gets no answer.
We try to mimic the situations they will find in real life, to make nursing tangible,” Hillier says. “You can’t plan a seizure in a clinical rotation. You can plan that in a sim lab.
“Help me,” Bernier mouths to classmates. Two students wheel over a bassinet, but the mom won’t put the baby down. The entire class exchanges confused glances.
That’s when Maureen Hillier, College of Nursing simulation educator and assistant clinical professor, enters the room, ending the mock nursing scenario and asking students to join her for a debriefing. She reveals that the “mom” is really junior nursing student Sara Kingsborough and the “baby” is a mannequin. The scenario was arranged to add a layer of realism to the College’s simulation laboratories, a critical component of nursing education.
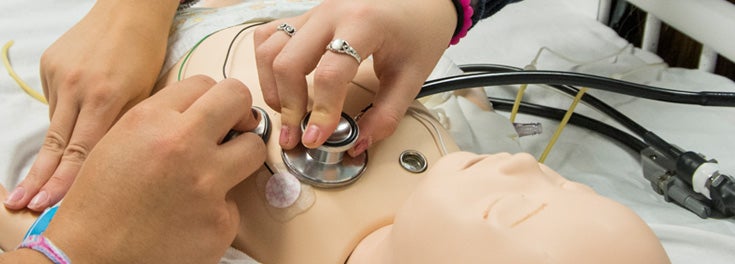
 This fall, nearly 100 freshmen got a first dose of the simulation labs, which are set up to mirror hospital settings, with a range of “patients” — interactive mannequins that cough, breathe, speak, cry, vomit, and exhibit vital sign changes. Although directed by an instructor, high-quality simulation also depends on Todd Madison, an instructional technology manager at the College, who drives the action from behind one-way glass in a darkened control room. The instructors monitor and assess students’ responses to scenarios.
This fall, nearly 100 freshmen got a first dose of the simulation labs, which are set up to mirror hospital settings, with a range of “patients” — interactive mannequins that cough, breathe, speak, cry, vomit, and exhibit vital sign changes. Although directed by an instructor, high-quality simulation also depends on Todd Madison, an instructional technology manager at the College, who drives the action from behind one-way glass in a darkened control room. The instructors monitor and assess students’ responses to scenarios.
Madison has spearheaded recent upgrades: acquiring more sophisticated mannequins, building wall dividers to impart a busy health-care setting, and streaming live simulation into the classroom. Sometimes he voices a “patient” from the control room.
“We want to crank the pressure up a bit. We can program in a medical error or have graduate assistants play the role of family members,” Madison says.
“It’s a very resource-intensive enterprise, and we want to do it well,” says Hillier, who led simulation education at Boston Children’s Hospital and remains on that faculty part time. She began teaching clinical rotations for URI nursing students at Children’s three years ago, and returned to URI this fall, introducing the actor component to simulation.
During the debriefing, students talk about feeling anxious when the baby mannequin went into cardiac distress and confusion when the young woman with the baby walked in.
“We push you to the edge of the cliff but we are never going to let you fall off. That’s where some of the best learning takes place,” Hillier tells the students later. “You can practice here in a safe environment. You are never graded on what happens here.”
The learning that takes place in the student-centered debriefing is as important as the simulation, she notes. One by one, the freshmen share what the unscripted experience taught them: Work together, be confident, pay attention, address a problem as soon as you see it, be kind—all valuable lessons for nursing in the real world.
