
From Assistant to Expert: Redefining Nursing
For 75 years, URI’s College of Nursing has been at the forefront of a changing profession.
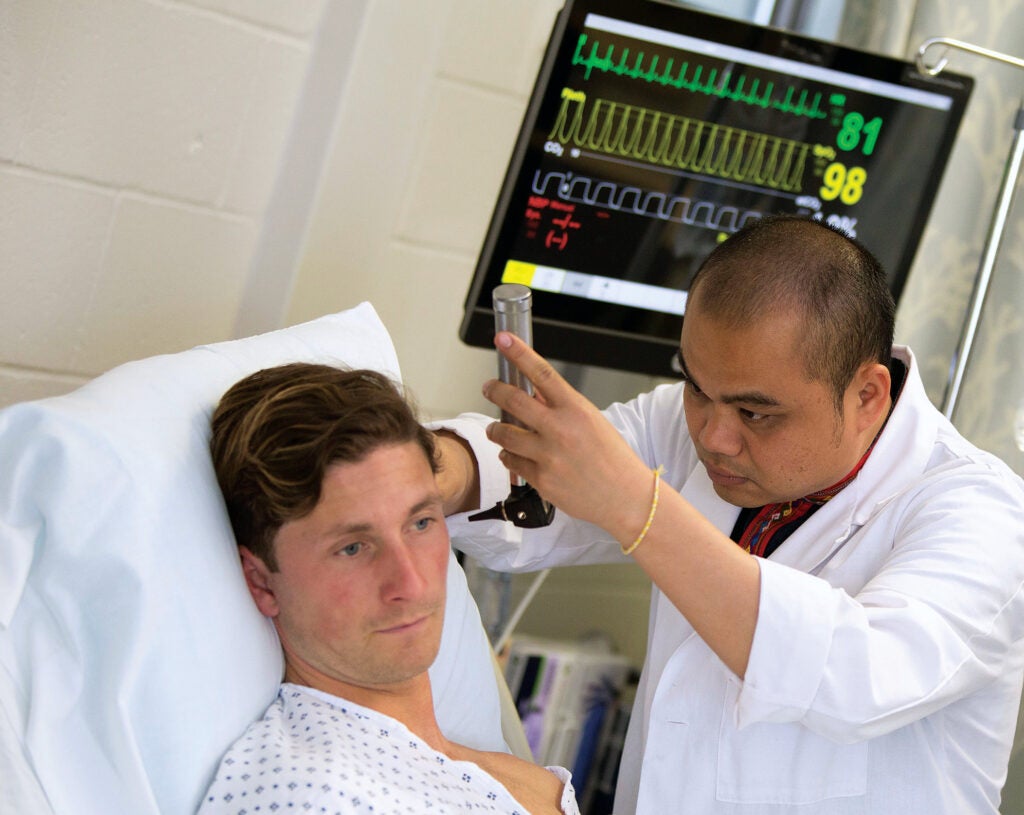
Experiential learning and clinical rotations are an important part of the curriculum for URI’s student nurses.
By Michael Blanding
For as long as she could remember, Diane Healey Dexter ’50 wanted to be a nurse. “I was always so pleased if any of my playmates had a splinter,” she chuckles, remembering her South County childhood. “They used to run away because they knew I’d want to practice on them.” When Dexter was searching for a registered nursing program after high school, however, all the hospital programs had a minimum age requirement of 18, and she was only 17. She decided to take a chance on a brand-new program at the University of Rhode Island.

In 1945, baccalaureate nursing programs were a novelty. Most nurses were educated at hospitals, focused on teaching routine tasks with a variable curriculum. Not until after World War II did the National Nursing Council call for more rigorous accredited university-based programs. At URI, that charge was led by Louisa White, the school’s first dean. “Louisa had the vision and the tenacity to say, ‘It’s time that nursing is a profession that is educated like a profession,’” says Barbara Wolfe, current dean of URI’s College of Nursing. “Women weren’t necessarily pursuing higher education opportunities—never mind a whole new career opportunity in a university setting.”
Dexter joined a group of eight students moving into Davis Hall for a five-year program of instruction and practical training in pediatrics, communicable diseases, diabetes, and other disciplines at area hospitals. “We had Quonset huts for recreational areas and you had to be in your room by 8:30,” she remembers. Despite such humble beginnings, she graduated in January 1950, part of a new generation of nurses confident to take on any challenge. After starting out in a hospital, Dexter spent much of her career working for Washington County, Rhode Island, assessing children born with developmental or cardiac problems.
“Decades ago, nursing was more of a support role to physicians. Now it is truly recognized as an independent profession.”
—Barbara Wolfe, Dean, URI College of Nursing
Over the past 75 years, nurses have risen far beyond the image of women in white caps and aprons changing hospital bedpans. They are now a diverse group with places in every aspect of the health-care arena—as administrators, research scientists, and bedside and primary-care clinicians. “Decades ago, nursing was more of a support role to physicians,” says Wolfe. “Now it is truly recognized as an independent profession.”
As doctors have become increasingly specialized, nurses have become the glue holding our medical system together—the only people with a holistic view of the patients they serve. Nothing has demonstrated this fact more than the coronavirus pandemic, which has thrust nurses onto the front lines, keeping patients alive even as they put themselves at risk.
In this age of COVID, as URI’s College of Nursing marks its 75th anniversary, its alumni reflect on their decades-long journey, even as they face their greatest challenge.
1960s and 1970s: Out of the Shadows

When Paula Viau ’69 was looking for a nursing program in 1965, her high school guidance counselor gave her some advice: “If you want to be a nurse, you need to go to college.” At that time, URI was one of only two baccalaureate programs in the state. “Going there was the best decision I ever made,” says Viau. “When I graduated, everyone immediately found clinical employment.” She began working at the state health department, before going on to become a URI professor and associate dean.
By the late 1960s, the school had grown to more than 30 students, but was still a tight-knit group. “We all supported each other,” remembers Elaine Riley ’68. “Whenever you had difficulties, somebody was always there to help you through it.” Under Dean Barbara Tate, URI was on the cutting edge of nursing practice, expanding beyond the hospital setting to increasingly venture into community care. Riley was captivated by the experience of entering patients’ homes to provide care in that intimate setting. “In home care, you see the whole thing—how they interact with their families, and their home environment,” she says.

Riley formed her own company to provide skilled and non-skilled home care to children and elderly patients—it grew into HomeCare Advantage, one of Rhode Island’s largest home nursing companies, with more than 200 employees. In 2011, she established a scholarship at URI for nursing students interested in community care, to pay for their last year of instruction. “You really need a well-educated nurse to do home care,” says Riley, who is semi-retired, running her company with her daughter. “It’s not like in a hospital where you can go and ask somebody if you don’t know something. Your nursing skills must be top-notch, and URI provides that quality education.”
By the mid-1970s, the “writing was on the wall” about the importance of a college nursing degree, says Dayle Joseph, who began teaching at URI in 1973, and was dean of the school from 1995 to 2012. “Everyone was saying you had to go the baccalaureate route.” By that time, URI had started a master’s program, and moved into its permanent home in White Hall, where it created state-of-the-art simulation labs that offered practice opportunities in hospitals, homes, and psychiatric units.

At the time, recalls Kristen Swanson ’75, career opportunities for young women were still limited. “You could be a nurse, a teacher, or an administrative assistant,” she says. She recalls an incredibly rigorous program—especially a dreaded anatomy class with Professor Robert DeWolf. “He had a commanding presence that left no room for weakness,” she says. “But in the end, what he taught us carried me for the rest of my career.”
In those days, Swanson says, nurses were subservient to physicians. “There was a lot of deference given to medicine,” she says. Since most doctors were men and nearly all nurses were women, she says, “sexism was a very strong experience.” But slowly, times were changing. Determined to grow in her profession, she earned her master’s degree at the University of Pennsylvania in 1978 and her Ph.D. at the University of Colorado in 1983, using both quantitative and qualitative methods to study the experience of miscarriage.
At the time, the health-care system often disregarded the emotional repercussions of miscarriage for women. In trying to understand how women wished to be responded to when they experienced early pregnancy loss, Swanson developed what is now known as the five-step Swanson Theory of Caring, consisting of five ways of relating to another human being—knowing, being with, doing for, enabling, and maintaining belief—that is still held up as the gold standard for care. “What gives me the greatest comfort is to know the work I did on miscarriage and caring has influenced practice and actually improved outcomes,” she says.

Later, when Swanson miscarried herself, she experienced firsthand what it was like to be on the other side of the science. “It’s a validation I never would have asked for, but after that, I didn’t need anyone to tell me I did good science—I could feel it in my heart.”
As part of the first generation of nurse-scientists, Swanson’s struggles were typical of nurses coming out of the shadow of medicine. “We were at the crossroads of whether we were really a discipline unto itself,” she says. “Was nursing truly science, or was it just some psychosocial softness?” Now, of course, the answer to that question is clear, says Swanson, a professor and dean of the College of Nursing at Seattle University, and chair of the Board of Trustees of Swedish Health Services. “I see so many good opportunities to expand clinical knowledge through qualitative work, quality improvement projects, and randomized controlled trials,” she says.
Besides sexism, the profession has also struggled with racism. A second-generation Cape Verdean from Cape Cod, Josepha Campinha-Bacote ’74 came to URI in 1970, and thrived under the example of Dean Tate and Professor Sylvia Blount, whom she found incredibly caring and knowledgeable. “I was inspired by that blend of humility and competence,” Campinha-Bacote says.

Campinha-Bacote struggled with questions of identity in her nursing career. As the granddaughter of immigrants from the islands of Cabo Verde (Cape Verde), off the coast of Africa, she felt apart from African-American culture. “I didn’t even know I was black at the time,” she says. Early in her life, however, she experienced the tragic consequences of cultural incompetence in the medical profession when her 78-year-old grandfather was prescribed a medication for cardiovascular issues. The medication came with the side effect of slowing the heart rate, and patients are not supposed to take it if their heart rate falls below a certain level. Raised on Cabo Verde without clocks, however, her grandfather was never told how to accurately time his pulse, and he died from complications taking the medicine.
Her personal loss illustrated a larger issue in health care: the failure of health-care professionals to understand the important difference between a language translator and a cultural interpreter. As a master’s student, Campinha-Bacote began developing a model for how health- care professionals can develop cultural competency, which she envisions as an ongoing process, starting with the humility she learned from her mentors at URI, transformed through cultural desire, awareness, knowledge, and skill. She coined the term “cultural competemility,” a portmanteau of “competence” and “humility,” to describe her own model of transcultural care.
By the late 1960s URI was on the cutting edge of nursing practice, expanding beyond the hospital setting to increasingly venture into community care.
Since developing her model in the early 1990s, she has written numerous books, and through her company, Transcultural C.A.R.E. Associates, has given more than 1,000 presentations to medical institutions, health-care organizations, and corporations such as Proctor & Gamble. Recently she has moved into more explicitly anti-racist work in order to challenge the assumptions that nurses apply to their patients. “People say the first step is cultural awareness, but at this point I think we are all aware that racial issues exist. It’s more about, ‘What actions are we taking?’”
1980s and 1990s: Into Their Own
The 1980s were a time of dramatic change in the health-care system. Cost pressures led hospitals to shift from a reliance on high-salaried doctors to lower-paid nurses for health-care services. That, in turn, created a higher demand, leading to a nationwide nursing shortage that gave nurses new bargaining power to push for higher wages and more independence. Gone were the caps and aprons—and in came the pantsuits—as nurses increasingly took a place as administrators. “Nurses are the people who really know their patients,” says Joseph, “and increasingly our voices were being heard.”

URI responded with new degree programs for nurse administrators and nurse practitioners, who take on many of the functions of medical doctors in diagnosing patients, prescribing treatments, and referring patients to specialists. “Nurse practitioners are well-educated and highly skilled,” says Joseph. “More importantly, patients have increased access to health care, as nurse practitioners have added significant numbers of health-care providers and have a proven record of successfully caring for patients.”
Some of those trends first started emerging in the military, says Daniel Wasneechak ’89, M.S. ’93, a New York native who first entered the profession as commissioned Nurse Corps Officer when he was an ensign in the Navy in 1976. “I absolutely loved the human touch, and the satisfaction of seeing the little things you could do to make someone’s life better,” says Wasneechak, who worked in an ICU and a cardiac surgical unit. While on active duty, he watched as nurses ran clinics on their own.
“The profession was evolving at the time, where nurses were no longer the handmaidens of the physicians,” Wasneechak says. As new wellness research emerged to connect physical and mental health, “we were really talking about how you could treat the whole patient, not just passing bedpans and changing bandages.” Enrolling at URI to advance his career, he was able to share his experiences in the military and learn about advancements in the civilian world. “URI allowed me to develop my own curriculum,” he says. “I already had many of the skillsets, but I needed more experience in leadership and administration.”
He continued on to earn a master’s degree in nursing at URI, followed by a master’s in health care administration at Baylor University. After working in a series of administrative positions, Wasneechak now oversees global quality with International SOS, the TRICARE Overseas Program, a government contractor providing health care to military personnel, their families, and retirees serving outside the United States. “I have regional quality managers who are nurses, and being able to talk the talk with them allows me to get buy-in much more quickly.”

In the ’80s, URI’s College of Nursing also launched a Ph.D. program and expanded its own research under the leadership of Hesook “Suzie” Kim, who was dean from 1983 to 1988. A researcher in the areas of nursing theory and collaborative decision-making, Kim encouraged faculty to increase their own research programs. These scholarly efforts were further enhanced by Dean Jean Miller, drawing on her experience as an associate dean for research at the University of Utah, where she served prior to her arrival at URI.
During this time, the school expanded its reach internationally, as well. Inger Magrethe Holter, M.S. ’87, Ph.D. ’93, was working as a nurse in Norway when Tate visited the country as a Fulbright scholar. Norway didn’t then have any nursing master’s programs, and Tate encouraged her to come to URI to earn her advanced degree. Holter came to Kingston for two years to earn her master’s, and returned again a few years later to earn her Ph.D., as well. She focused her efforts on “action research,” a new method involving collaboration between academics and practitioners to bridge the gap between theory and practice. Holter wrote an influential paper on the topic in 1993.
Returning to Norway, she taught as a professor at the University of Oslo, and became chief nurse at the university-affiliated hospital, the first nurse with a Ph.D. to serve as a hospital administrator in Norway. The collaboration between URI and Norway continued as Kim became a visiting professor at the University of Oslo, sharing research data and increasing cross-cultural exchange between the two campuses. When Holter became dean at Buskerud University College in Drammen, Norway, she asked Kim to come help her launch a master’s program. “She did so much to build up nursing master’s and Ph.D. programs in Norway,” Holter says. “URI has been so important for Norway in establishing the higher education we have today.”
Nursing continued to struggle with issues of diversity in a profession that was traditionally young, female, and white. By 1990, only 11 percent of nurses were people of color, compared to some 30 percent of the population—the result of a long history of segregation and discrimination in health care. It wasn’t easy for those looking to reverse those trends, says Laitan Silifat Mustapha ’97, a Providence native born of first-generation Nigerian parents.
“Nurses have a lot of say in the care of their patients, because we’re with them for a much longer time.”
—Laitan Silifat Mustapha
Laitan Silifat Mustapha ’97 is vice president of nursing for Unity Health Care in Washington, D.C.
“Nursing school was very difficult for me,” says Mustapha, who was recruited to URI through Talent Development, a program for high school students from underserved populations. While the program provided an advisor and tutoring to get into college, once at URI, she felt adrift among the nursing school’s largely white student body and faculty.
“I didn’t have any professor who understood where I was coming from and could relate to me,” says Mustapha, who had to repeat classes, and was in danger of failing. “I think white people don’t understand that, since they are so used to seeing people who look like them.” She persevered, however, and when she started working at Rhode Island Hospital after graduation, an African-American nurse on her floor took her under her wing and helped her succeed. “She was a great mentor—she told me specifically she did not want me to fail.” Later, she moved to Maryland, where she not only regularly saw nurses of color, but saw them in high-level positions.
By 1990, only 11 percent of nurses were people of color, compared to some 30 percent of the population—the result of a long history of segregation and discrimination in health care.
Mustapha earned a master’s at Benedictine University and is currently studying for her Ph.D. at Catholic University in Washington, D.C. Now, she is vice president of nursing for Unity Health Care, a nonprofit network of community health centers in Washington, D.C., that serves a high-risk population. “You have to understand not only their physical limitations, but their social needs and mental health needs as well,” Mustapha says. Much of that responsibility falls on nurses, who, more than doctors, follow patients intimately throughout their care. “Nurses have a lot of say in the care of their patients, because we’re with them for a much longer time.”
As health insurance has expanded medical access to a broader population, including more minorities, Mustapha adds that it’s even more important that nursing schools recruit faculty and students who reflect the diversity of the population. While some progress has been made on diversifying nursing ranks, currently only 19 percent of nurses are people of color.
At URI, Wolfe says increasing diversity is a major objective in the nursing school’s current strategic plan. In 2010, the college launched its Pathways to Nursing program, which provides tutoring and social support to students from disadvantaged backgrounds. In her four years as dean, Wolfe has also worked to diversify the faculty, increasing the number of full-time faculty members of color from one to four (out of a total of 36) over that time. “We’re actively recruiting, and starting to make incremental progress,” she says.
The Pathways to Nursing Program was launched in 2010 to recruit, support, retain, and graduate educationally, economically and socially disadvantaged students. Pathways students gathered at the annual Pathways Living Leadership reception in December 2018. Program administrator Professor Mary Cloud in back on left; Associate Dean Mary Leveille in back, second from left; Dean Barbara Wolfe in back, second from right.
2000s and 2010s: In the Spotlight

The turn of the century saw another nursing shortage, as baby boomers began to retire, and the health-care system relied on nurses more than ever. As knowledge and technology have improved, care has increasingly moved out of hospitals and into primary-care and community settings, where nurses are apt to be the patient’s main conduit to health. “Hospitals are not where most people receive care anymore,” says Wolfe. “We need to make sure we have clinicians who are truly able to meet the need for appropriate care in those non-hospital settings.”
In response, the types of degrees nursing schools offer have exploded. URI created a range of specializations in its graduate program, including family, gerontology, and psychiatric mental health nursing. The school has also continued to make its mark in research. In the late 1980s, Professor Margaret McGrath started studying a cohort of babies with low birth weight; more than 20 years later, in 2011, her successor, Professor Mary Sullivan, tied premature birth to a range of health and social struggles in adulthood—as well as pointing to factors to minimize those issues. In 2016, URI professors Judith Mercer and Deb Erickson-Owens were able to show that delaying clamping of the umbilical cords of newborns by even five minutes dramatically improved outcomes, setting a new standard for obstetric practices.
As knowledge and technology have improved, care has increasingly moved out of hospitals and into primary-care
and community settings, where nurses are apt to be the patient’s main conduit to health.
Mary-Ellen Doherty, Ph.D. ’00, came to URI as a graduate student after a successful career as a nurse-midwife. Using theories of collaborative decision-making pioneered by Suzie Kim, she examined how nurse-midwives and clients can best formulate a birth plan. Amid that research in the early 2000s, she interviewed women who had recently lost their spouses in the 9/11 terrorist attacks, or the wars in Iraq and Afghanistan, and focused her later research on exploring their stories using qualitative methods. “You are asking people to open up their hearts and minds and souls, to really tell you what their struggles are,” Doherty says, “what it’s really like to go through a pregnancy, labor, and birth without your person.”
War continued to influence her studies as Doherty began teaching at the University of Massachusetts–Lowell, and she saw multiple students in the National Guard or ROTC programs deploy for their first nursing assignment in a war zone. Doherty began interviewing nurses upon their return about their experiences. Now a professor at Western Connecticut State University, she has authored two books with her twin sister, a retired Air Force colonel: Nurses In War: Voices from Iraq and Afghanistan in 2012, and Nurses After War: The Reintegration Experience of Nurses Returning from Iraq and Afghanistan in 2016.
Not surprisingly, Doherty found many nurses struggling to overcome post-traumatic stress disorder (PTSD) upon their return. “They were able to manage over there, but then when they got home it hit them like a ton of bricks,” Doherty says. However, she also found a significant number who were transformed in positive ways by the experience. Doherty is now expanding her research to look at the concept of post-traumatic growth in people who have survived traumatic experiences, such as war, abuse, or the loss of a loved one. “There can be some growth and greater appreciation of life—you don’t often read about that.”
In 2017, the college opened a new Nursing Education Center, a $220 million 133,000-square-foot building in Providence with new classrooms, labs, and simulation rooms. “It’s an amazing building that has the same kind of equipment you would see in maternity, pediatric, or medical/surgical units,” says Viau. The building became headquarters for the college’s graduate programs—including a new Doctor of Nursing Practice degree, a terminal to prepare experts in specialized advanced nursing practice.
The Nursing Education Center at South Street Landing in Providence is home to the college’s graduate programs and to new classrooms, labs, and simulation rooms.
URI nursing students get hands-on practice in a simulation lab in the Nursing Education Center.
One of the first recipients, Colin Burns ’14, D.N.P. ’19 originally planned to be a physician, but realized that he could have more opportunities for developing relationships with patients as a nurse practitioner. “As the future of medicine seems to be focusing on specialization, nurse practitioners are really stepping up to meet the moment to fulfill that primary care role,” says Burns. In pursuing his undergraduate degree at URI, Burns initially focused in pediatrics; but after a rotation in the geriatric ward at Butler Hospital in Providence, he chose the opposite end of the spectrum, specializing in geriatric psychiatry, instead.

“I absolutely fell in love with the population,” he says. “They have such great life histories and life lessons.” To better work with the population, he stayed at URI to earn his D.N.P., before helping to open a new inpatient geriatric psychiatric unit at Yale New Haven Health Westerly Hospital as lead nurse practitioner. “The leadership skills I learned at URI really helped in being on the ground floor at the unit’s opening,” he says. “In setting up a practice environment, I was able to focus on how we can do things better and more efficiently.”
Those practices have been put to the test this past year during the coronavirus pandemic, to which elderly patients have been particularly susceptible. “We’re seeing so much of the older population affected by the social isolation,” Burns says. “It’s caused an increase in depression that has just been heartbreaking.” Last March, his unit was at the forefront of requiring mandatory COVID testing for patients before admission—now standard practice at many hospitals—so patients could freely socialize with one another once they were admitted. “Knock on wood, we haven’t had any cases, and I think a lot of that has been due to proactive management,” Burns says.
“As the future of medicine seems to be focusing on specialization, nurse practitioners are really stepping up to meet the moment to fulfill that primary care role.”
—Colin Burns ’14, D.N.P. ’19
The pandemic has strained the capacity of nurses all over the country. “Nurses have been stressed out, worried, and afraid,” says Mustapha. “We’ve really bonded together in this moment.” To keep up morale of those under her care, she has increased site visits to ensure communication, and has implemented weekly meetings over Zoom to check in with managers. “I have been able to empower them to make their own decisions in the best interest of themselves and their patients.” That includes a more lenient absence policy for nurses who have needed to take breaks or work remotely, and allowing nurses to determine when it’s safe, for example, to open a mobile tent for testing.
In Rhode Island, nurses have been both on the front lines in the ICUs, and directing the highest levels of the state’s response. “Years ago, nurses weren’t at the head table making decisions,” says Joseph. Now, she says, URI graduates are regularly on television as the public face of the crisis response, including Cathy Duquette ’83, M.S. ’96, vice president and chief nursing officer at Lifespan, the state’s largest medical organization, which manages Rhode Island Hospital and has set up a 600-bed field hospital for COVID patients in Providence. Joseph is, herself, a governor at the Miriam Hospital in Providence, where, in January, URI nursing alumna Maria Ducharme, M.S. ’95, became president—the first time in that hospital’s 95-year history that it promoted a nurse to its highest leadership position.

At URI’s College of Nursing, faculty and students have also been struggling with the new realities of the pandemic, embracing distance learning to teach students. “That becomes a difficult task when it’s so important to have that one-on-one connection in clinical settings,” says Viau. “I’m sure 10 years from now, faculty will look back and say this was the biggest challenge we’ve ever undergone.” The current situation has already impacted the curriculum, emphasizing the need for nursing students to be fluent in telehealth, which is apt to outlive coronavirus as an efficient tool for reaching patients.
One perhaps surprising result of the pandemic has been an increase in applications for admission to the College of Nursing, says Wolfe. At a time when nurses are literally risking their lives to treat a deadly infectious disease, she’s been proud to see a new contingent of future nurses eager to do their part in furthering the health of Rhode Island and beyond. “These are people who are truly interested in a career built out of helping others and bettering society,” Wolfe says. “It’s reassuring, quite frankly, to know there are people out there who are willing to put themselves in those situations to help the less fortunate.”
In December, Time magazine readers voted nurses and other frontline workers their “Person of the Year” in a reader’s poll.
Even before the pandemic, in January 2020, Americans rated nurses as the most trusted profession for the 18th year in a row, with 85 percent ranking their honesty and ethics “very high.” In December, Time magazine readers voted nurses and other frontline workers their “Person of the Year” in a reader’s poll. As the country recovers from the pandemic, nurses are bound to become only more prominent as the face of health-care delivery. It will remain up to schools like URI’s College of Nursing to continue preparing them for the next national challenge: adapting to the broad transformation—and the day-to-day challenges—of health care in the coming decades.
Mustapha compares nurses emerging from the pandemic to a scene in an action movie where people walk out of an explosion, disheveled, perhaps, but defiant and alive. “Everyone has the choice about whether to flee or fight,” she says. “Those of us who have stayed in this profession are going to come out of this stronger and more resilient, able to handle anything that comes our way.” •
Photos: Nora Lewis; URI College of Nursing; Courtesy Josepha Campinha Bacote; Colin Burns; Diane Healey Dexter; Mary-Ellen Doherty; Inger Magrethe Holter; Dayle Joseph; Patrick Luce; Laitan Silifat Mustapha; Kristen Swanson; ; Paula Viau; Daniel Wasneechak

I was on the faculty for many years and was disappointed that the nursing school never ranked nationally. One of the big problems was the multi hiring of part time clinical faculty who never integrated themselves into the college. They had much lower standards for students. Most of the graduate faculty stayed too long.